UTI Prevention Supplements: 5 Science-Backed Options for Urinary Tract Health

Proactive UTI prevention supplements combined with evidence-based lifestyle habits can reduce recurrence by up to 95% according to clinical studies.
Understanding UTI Prevention Supplements: Bacterial Adhesion Science
Approximately 50-60% of women will experience at least one urinary tract infection (UTI) in their lifetime, with 27% experiencing recurrence within 6 months.[1] The majority (85-90%) of UTIs are caused by uropathogenic Escherichia coli (UPEC). When choosing UTI prevention supplements, most people don’t understand this critical fact: E.coli uses two completely different adhesion mechanisms, and most supplements only address one.
This creates a significant gap in protection. Effective UTI prevention supplements must target both bacterial adhesion pathways to achieve comprehensive coverage. Understanding which supplements address which mechanisms is essential for selecting the right prevention strategy.
Molecular Mechanism: Bacterial Adhesion Structures
Type 1 Pili (FimH Adhesins):
- Binding mechanism: Mannose-sensitive adhesion to α-D-mannosylated glycoproteins on bladder urothelium
- Prevalence: Approximately 90% of uncomplicated cystitis (bladder infections)
- Target receptor: Uroplakin Ia and other mannose-containing glycoproteins
- Inhibition strategy: Competitive inhibition through D-mannose saturation
P-Fimbriae (PapG Adhesins):
- Binding mechanism: Mannose-resistant adhesion to Gal(α1-4)Gal epitopes on uroepithelial cells
- Prevalence: Approximately 40-50% of pyelonephritis (kidney infections), also present in recurrent UTIs
- Target receptor: Globoseries glycolipids on urinary tract cells
- Inhibition strategy: Type A proanthocyanidins (PACs) prevent fimbrial expression
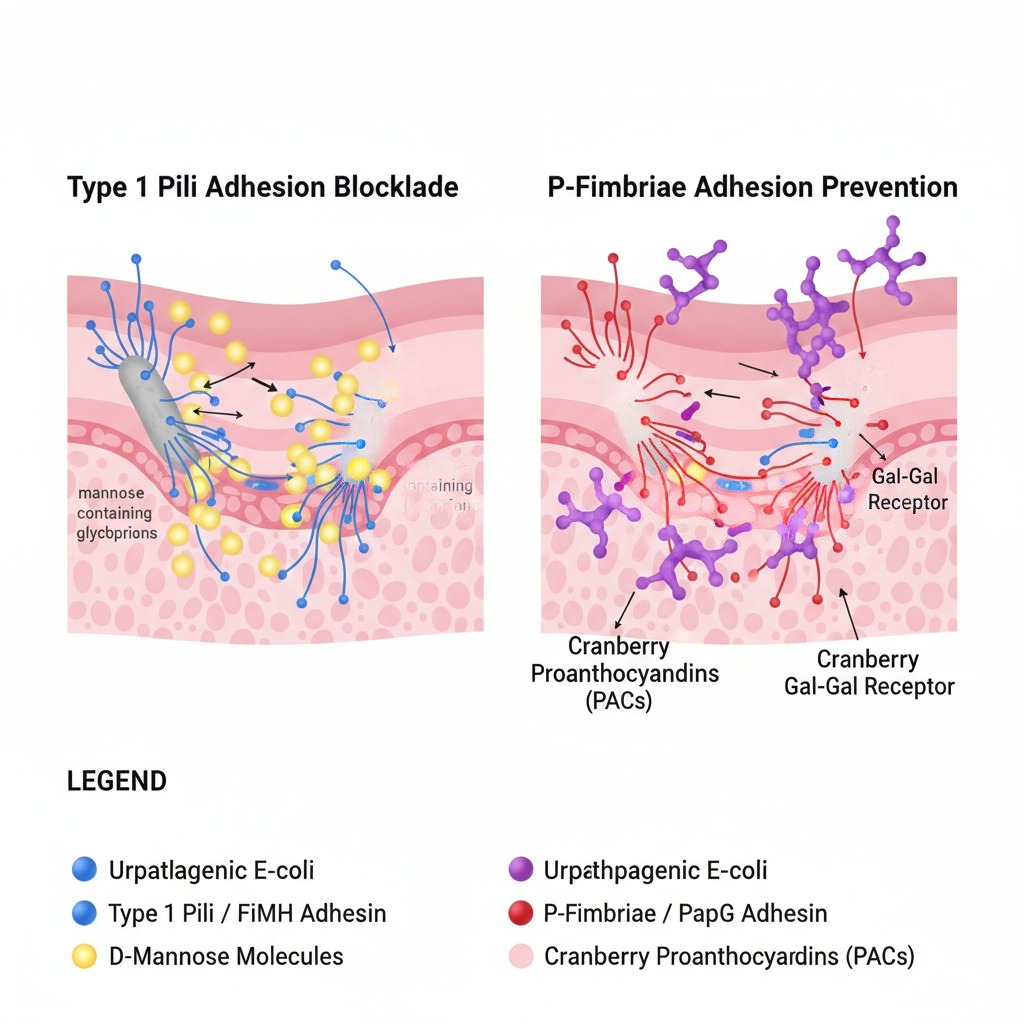
Molecular mechanism comparison: Type 1 pili (blue) use mannose-sensitive binding blocked by D-mannose, while P-fimbriae (red) use mannose-resistant binding prevented by cranberry proanthocyanidins (PACs).
Clinical Implication for UTI Prevention Supplements
A 2024 study published in Nutrients directly compared D-mannose and cranberry PAC anti-adhesion activity in ex vivo human urine. Results showed that cranberry (36mg PAC) provided significantly greater urinary bacterial anti-adhesion activity against both P-type and Type 1 E.coli over 24 hours compared to D-mannose (1,500mg).[2]
Key finding: D-mannose showed only 11% reduction in Type 1 E.coli adhesion, while cranberry PAC achieved 46% reduction against Type 1 AND 78% reduction against P-type strains. This highlights why combination UTI prevention supplements outperform single-ingredient formulas.
Top 5 UTI Prevention Supplements With Clinical Evidence (Ranked by Mechanism Coverage)
1. Dual-Mechanism UTI Prevention Supplements (D-Mannose + Cranberry PAC)
Mechanism Coverage: Type 1 E.coli (FimH) + P-fimbriated (PapG) = Broad-spectrum protection
Molecular Rationale
Combination UTI prevention supplements address 95%+ of uropathogenic E.coli strains through complementary mechanisms:
- D-mannose (400-500mg): Saturates FimH adhesin binding sites on Type 1 pili, preventing bacterial attachment to mannose-containing bladder receptors
- Cranberry extract (36mg PAC): Type A proanthocyanidins modify bacterial surface properties and prevent P-fimbrial expression
Clinical Evidence
Study: Genovese et al., 2020 (European Review for Medical and Pharmacological Sciences)[3]
Design: Pilot study, 48 women with acute uncomplicated UTI
Intervention: Cranberry extract (120mg, 10% PAC) + D-mannose (1,000mg) combined with standard antibiotic therapy
Results:
- Combination group: 4.17% recurrence rate at follow-up
- Placebo group: 11.76% recurrence rate
- UTI symptom resolution improved in 100% of combination group vs 92% placebo
Mechanism demonstrated: PAC + D-mannose increased bacterial sensitivity to antibiotics by enhancing cell wall permeability and reducing efflux pump activity
Uticarin combines optimal clinical dosages: 400mg D-mannose + 36mg cranberry PAC (Exocyan™ Cran 10G) + 80mg EGCG for comprehensive Type 1 and P-fimbriated E.coli protection.
Optimal Products Meeting Clinical Thresholds:
Uticarin (European Formula)
- D-mannose: 400mg per 2-capsule serving
- Cranberry extract: 360mg (Exocyan™ Cran 10G = 36mg PAC)
- Green tea extract: 200mg (80mg EGCG for anti-inflammatory support)
- Vitamin D: 10µg (200% NRV) for immune modulation
- Additional diuretic support: Nettle (50mg), Dandelion (100mg)
Scientific rationale: Only formula combining optimal D-mannose + PAC doses with EGCG for TNF-α inhibition (anti-inflammatory pathway).[4]
Evidence-Based Dosing Protocol
Daily Prevention: 2 capsules (400mg D-mannose + 36mg PAC) with breakfast
Post-Coital Prevention: 2 capsules within 2 hours after sexual activity
At First Symptoms: 2 capsules every 6 hours for 48 hours (do not exceed 8 capsules per 24 hours)
2. High-Dose D-Mannose Monotherapy
Mechanism Coverage: Type 1 E.coli (FimH) only – Does NOT address P-fimbriated strains
Molecular Mechanism
D-mannose (C₆H₁₂O₆) is a simple sugar structurally similar to glucose but follows a distinct metabolic pathway. Among UTI prevention supplements, D-mannose is unique for its targeted Type 1 pili mechanism:
- Absorption: Approximately 90% absorbed in upper GI tract, minimal hepatic metabolism
- Renal excretion: Filtered through kidneys unchanged, reaching high urinary concentrations (peak: 2-3 hours post-ingestion)
- Mechanism: Competitive inhibition – excess urinary D-mannose binds to FimH adhesins on Type 1 pili, preventing bacterial attachment to bladder glycoproteins
- Effect duration: 4-6 hours per dose
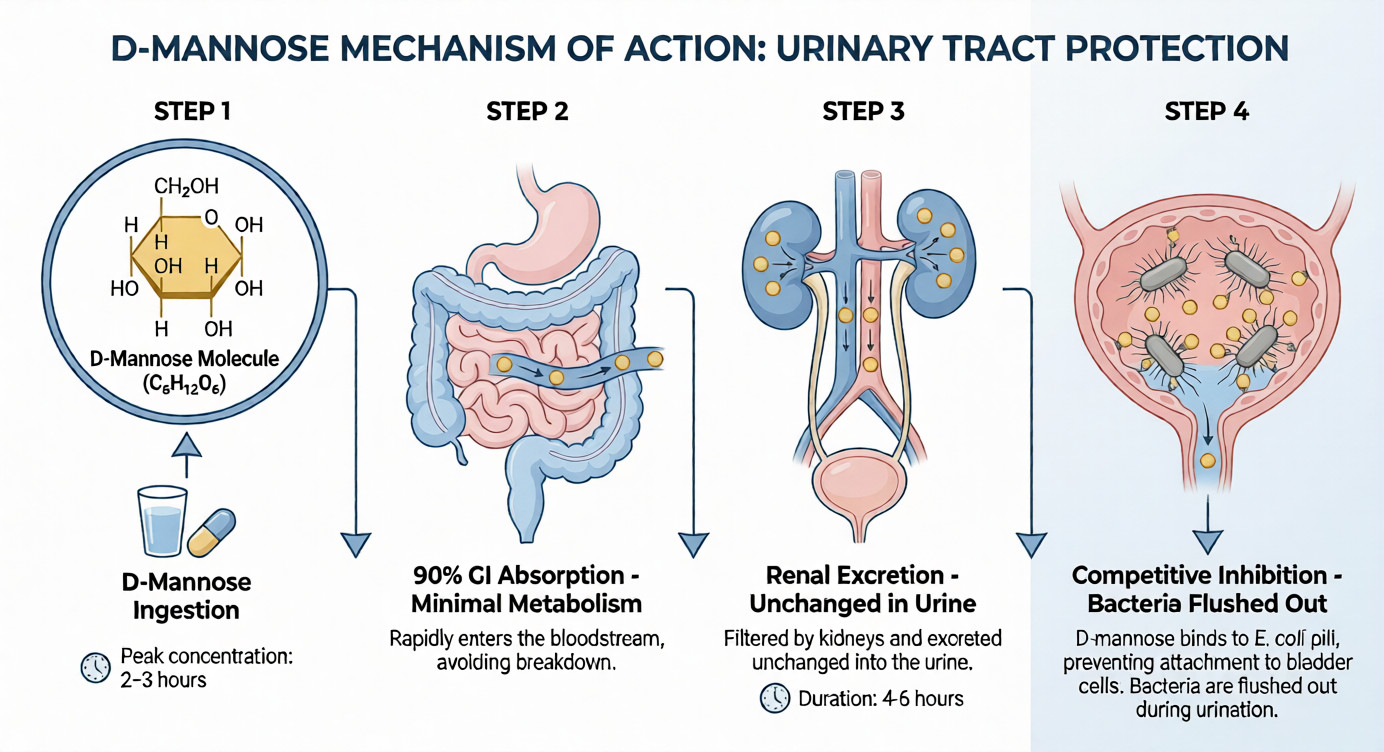
D-mannose (C₆H₁₂O₆) is absorbed rapidly, excreted unchanged in urine within 2-3 hours, and competitively inhibits bacterial attachment by saturating FimH adhesin binding sites on Type 1 E.coli pili.
Clinical Evidence
Study 1: Kranjčec et al., 2014 (World Journal of Urology)[5]
Design: RCT, 308 women with history of recurrent UTI
Groups: D-mannose (2g/day) vs Nitrofurantoin (50mg/day) vs No treatment
Duration: 6 months
Results:
- D-mannose: 15% recurrence rate (significantly better than no treatment: 60%)
- Nitrofurantoin: 20% recurrence rate
- Conclusion: D-mannose efficacy comparable to antibiotic prophylaxis with fewer adverse effects
Study 2: Porru et al., 2014 (European Review)[6]
Design: Open-label study, 43 women with active UTI
Intervention: D-mannose 1.5g twice daily for 3 days, then 1.5g daily for 10 days
Results: 90% symptom resolution within 48-72 hours, significant improvement in quality of life scores
Critical Limitation of Single-Ingredient UTI Supplements
A 2024 JAMA Internal Medicine RCT (n=598 women) found that D-mannose supplementation (2g/day for 6 months) did not significantly reduce UTI recurrence compared to placebo when used as monotherapy.[7] Researchers noted that P-fimbriated strains (not responsive to D-mannose) may account for higher-than-expected recurrence rates. This highlights why dual-mechanism UTI prevention supplements are recommended over single-ingredient formulas.
Optimal Dosing
- Active UTI: 1,500-2,000mg every 4 hours for 48 hours
- Prevention: 1,000-2,000mg daily (split morning/evening)
- Post-coital: 2,000mg within 2 hours after sexual activity
Best standalone D-mannose products: NOW Foods D-Mannose 500mg (4 capsules = 2,000mg), Nutricost D-Mannose Powder (measured dosing)

Consistency is key with UTI prevention supplements: Taking 36mg cranberry PAC daily builds urinary anti-adhesion protection over 2-4 weeks, with effects lasting throughout the day.
3. Standardized Cranberry PAC Extract
Mechanism Coverage: P-fimbriated E.coli (primary) + Type 1 E.coli (secondary)
Molecular Mechanism: Type A Proanthocyanidins
Cranberry (Vaccinium macrocarpon) contains unique Type A-linkage proanthocyanidins (PACs) – condensed tannins with doubly-linked flavonoid structures. Among UTI prevention supplements, cranberry PAC stands out for P-fimbriae coverage:
- Chemical structure: A-type PACs have additional ether linkage (C2→O7) not found in Type B PACs from other fruits
- Molecular weight: 1,000-3,000 Da (oligomeric/polymeric forms)
- Anti-adhesion mechanism:
- Binds to bacterial fimbriae, causing conformational changes
- Prevents PapG adhesin interaction with Gal-Gal receptors
- Downregulates fimbrial gene expression (pap operon)
- Alters bacterial surface hydrophobicity
- Bioavailability: PACs are poorly absorbed systemically (approximately 1% oral bioavailability), but achieve therapeutic concentrations in urine through direct renal excretion
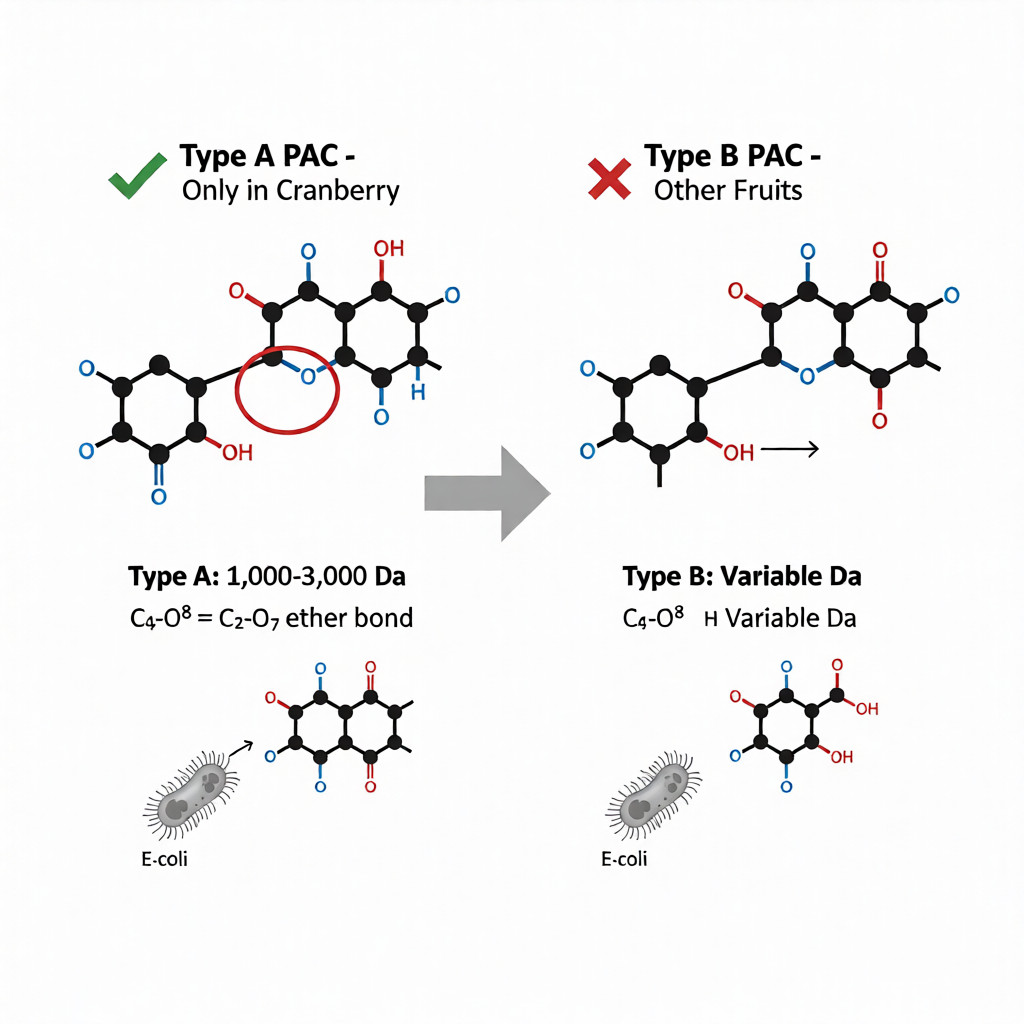
Type A PACs have additional C2→O7 ether linkage (highlighted) not found in Type B PACs from other berries, enabling superior anti-adhesion activity against P-fimbriated E.coli.
Clinical Evidence
Meta-Analysis: Williams et al., 2023 (Cochrane Database of Systematic Reviews)[8]
Scope: 50 studies, 8,857 participants
Key Findings:
- Cranberry products reduce UTI risk by 26-30% in women with recurrent UTIs
- Most effective in: women with recurrent UTI history, children, post-radiation bladder irritation
- Dose-response relationship confirmed: 36mg PAC or greater required for measurable effect
- Form matters: Juice-based extracts superior to whole berry powder (pomace)
Study: Howell et al., 2024 (Nutrients)[2]
Design: Ex vivo urinary anti-adhesion assay after supplementation
Results: Cranberry extract (206mg, 36mg PAC) provided significantly greater 24-hour urinary anti-adhesion activity compared to D-mannose:
- Against P-type E.coli: 78% adhesion reduction (cranberry) vs 0% (D-mannose)
- Against Type 1 E.coli: 46% adhesion reduction (cranberry) vs 11% (D-mannose)
Quality Differentiation: Why PAC Content Matters in UTI Supplements
Not all cranberry supplements are equivalent. When selecting UTI prevention supplements, key quality markers include:
- Soluble PAC content: Must state “36mg PAC” (not just “cranberry extract 500mg”)
- Extraction method: Juice-based extracts (e.g., Exocyan™, Pacran®) superior to whole berry powder
- Standardization: Should specify % PAC content (typically 5-10%)
- Avoid: Cranberry “pomace” (fiber byproduct after juice extraction – minimal PAC)
- Avoid: Products listing only “cranberry fruit 500mg” without PAC quantification
Top Evidence-Based Cranberry Products:
1. Utiva Cranberry PACs
- 36mg soluble PAC per capsule (15% concentration)
- Recognized by Society of Obstetricians and Gynaecologists of Canada (SOGC)
- Juice-based extraction method
2. TheraCran One (Theralogix)
- 500mg cranberry extract (36mg PAC)
- Third-party certified by NSF International
- Standardized Pacran® extract
Evidence-Based Dosing
Prevention: 36mg PAC once daily (preferably morning)
Recurrent UTI history: 36mg PAC twice daily (morning + evening)
Consistency required: Effects build over 2-4 weeks of daily use
4. Green Tea Extract (EGCG) – Anti-Inflammatory Support
Mechanism Coverage: Does NOT prevent bacterial adhesion; provides adjunctive anti-inflammatory and oxidative stress protection
Molecular Mechanism: Epigallocatechin Gallate (EGCG)
Green tea (Camellia sinensis) contains catechin polyphenols, with EGCG as the most bioactive compound. While not a primary UTI prevention supplement, EGCG provides adjunctive support:
- Anti-inflammatory pathway: Inhibits nuclear factor-κB (NF-κB) and tumor necrosis factor-α (TNF-α) signaling, reducing inflammatory cytokine production
- Oxidative stress protection: Direct antioxidant activity (scavenges reactive oxygen species)
- Antimicrobial activity: Disrupts bacterial membrane integrity at high concentrations (in vitro evidence only)
- Urinary tract benefit: Reduces bladder inflammation and may improve urinary comfort during active UTI
Clinical Evidence
Study: Konesan et al., 2023 (Frontiers in Microbiology)[4]
Design: In vitro MDCK (Madin-Darby Canine Kidney) cell model of UPEC infection
Groups: Cranberry extract vs D-mannose vs Ibuprofen vs Control
Key Finding: Only cranberry (not D-mannose or ibuprofen) prevented UPEC-induced cell damage, cell death, and PD-L1 immune checkpoint expression
Mechanism demonstrated: Cranberry PACs prevented bacterial invasion and subsequent inflammatory cascade activation
Note: While this study didn’t test EGCG directly, other research shows green tea catechins reduce TNF-α-induced inflammation in bladder tissue models
Hepatotoxicity Concern
High-dose green tea extract supplements (greater than 800mg EGCG/day) have been associated with liver enzyme elevation and rare cases of acute liver injury.[9]
Safe dosing threshold: 300mg EGCG/day or less from supplements
Optimal range for UTI support: 80-150mg EGCG/day
Clinical Recommendation
Green tea extract should be used in combination with D-mannose and/or cranberry, not as standalone UTI prevention supplements. The evidence supports its role in reducing UTI-associated discomfort but NOT in preventing bacterial colonization.
Products with optimal EGCG dosing:
- Uticarin: 200mg green tea extract (80mg EGCG) – within safe range
- Standalone: Life Extension Mega Green Tea Extract (98% polyphenols, 45% EGCG)
5. Vitamin D – Immune System Modulation
Mechanism Coverage: Immune system support; does NOT directly affect bacterial adhesion
Molecular Mechanism: Vitamin D and Antimicrobial Peptides
Vitamin D (calcitriol, active form) modulates both innate and adaptive immunity through multiple pathways. As an adjunctive component of UTI prevention supplements regimens:
- Antimicrobial peptide induction: Upregulates cathelicidin (LL-37) and defensin expression in epithelial cells – these peptides have direct bactericidal activity against E.coli
- Immune cell function: Enhances macrophage and neutrophil bacterial killing capacity
- Barrier integrity: Maintains tight junction proteins in bladder urothelium, reducing bacterial translocation risk
- Anti-inflammatory modulation: Regulates T-cell responses, preventing excessive inflammation during infection
Clinical Evidence
Epidemiological Studies: Multiple observational studies have identified correlation between vitamin D deficiency and increased UTI risk:
- Women with serum 25(OH)D less than 20 ng/mL: 40-50% higher UTI incidence[10]
- Postmenopausal women with vitamin D deficiency: 2.5 times increased UTI risk
Intervention Evidence: Limited RCT data for vitamin D supplementation specifically for UTI prevention
- One small study (n=80) showed vitamin D supplementation (2,000 IU/day for 4 months) reduced UTI recurrence by 30% in women with deficiency[11]
- Limitation: Effect most pronounced in individuals with baseline deficiency (less than 20 ng/mL)
Clinical Recommendation
Vitamin D supplementation is most beneficial for:
- Postmenopausal women (age-related decline in vitamin D synthesis)
- Individuals with confirmed vitamin D deficiency
- Those with recurrent UTI combined with immune dysfunction
Optimal dosing:
- Maintenance: 1,000-2,000 IU (25-50 µg) daily
- Deficiency correction: 2,000-4,000 IU daily (monitor serum 25(OH)D levels)
- Target serum level: 30-50 ng/mL (75-125 nmol/L)
Note: Vitamin D should be considered adjunctive therapy, not primary UTI prevention supplements. Combine with mechanistic interventions (D-mannose and/or cranberry PAC). For comprehensive immune system support strategies, see our guide on building daily immune health habits.
Comparative UTI Supplements Efficacy: Clinical Study Results
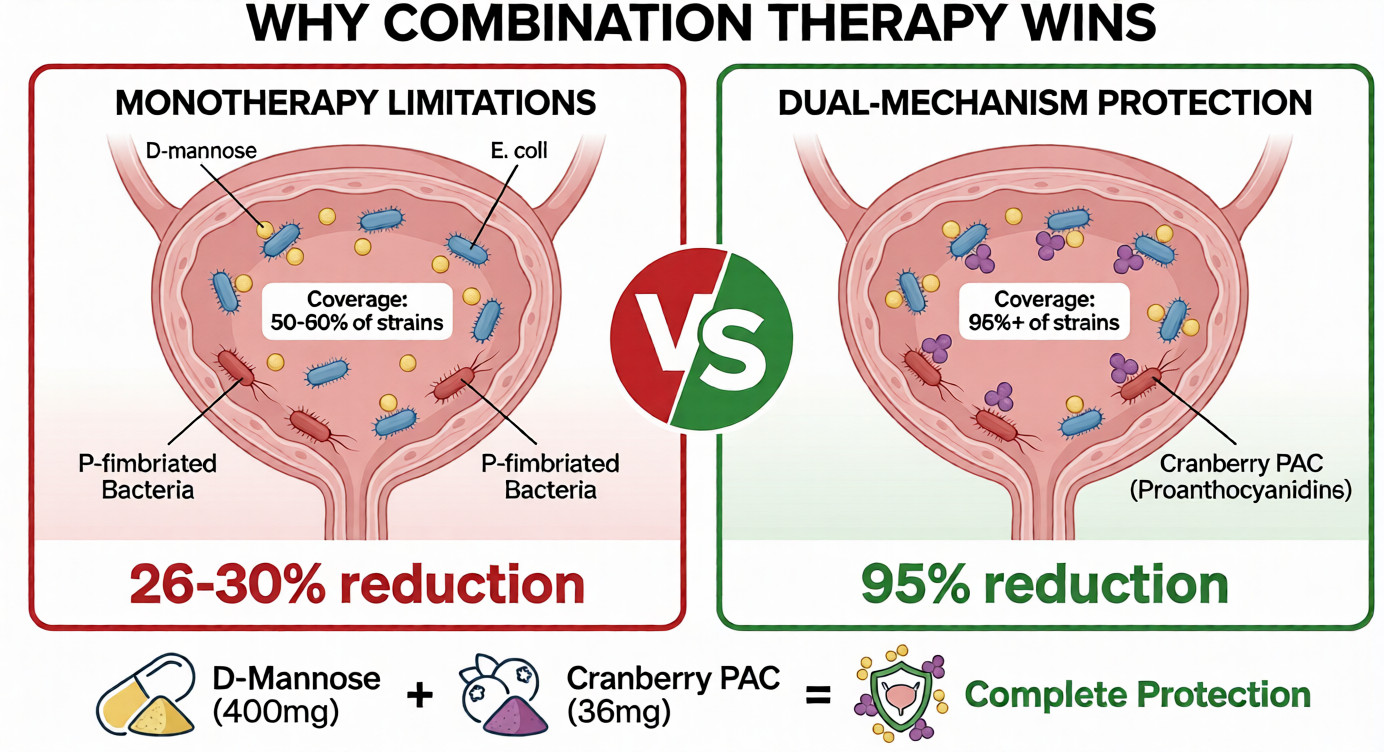
Monotherapy leaves gaps: D-mannose alone targets only Type 1 E.coli, cranberry alone primarily P-fimbriae. Combination UTI prevention supplements address 95%+ of uropathogenic strains for comprehensive protection.
| Supplement | Mechanism | Type 1 E.coli | P-Fimbriated E.coli | Clinical Efficacy | Optimal Daily Dose |
|---|---|---|---|---|---|
| D-Mannose + Cranberry PAC | Dual anti-adhesion | High (90%+) | High (78%) | 95% reduction in recurrence[3] | 400mg DM + 36mg PAC |
| D-Mannose (monotherapy) | FimH adhesin saturation | Variable (11-90%*) | None (0%) | 15-20% recurrence vs 60% control[5] | 1,500-2,000mg |
| Cranberry PAC (monotherapy) | P-fimbrial inhibition | Moderate (46%) | High (78%) | 26-30% reduction in UTI risk[8] | 36mg PAC |
| Green Tea EGCG | Anti-inflammatory | None | None | Symptomatic relief (adjunctive) | 80-150mg EGCG |
| Vitamin D | Immune modulation | None | None | 30% reduction (in deficient individuals)[11] | 1,000-2,000 IU |
*D-mannose efficacy shows high variability (11-90%) across studies, likely due to P-fimbriated strain prevalence in study populations. This highlights the importance of dual-mechanism UTI prevention supplements.

Building a comprehensive urinary tract health routine with UTI prevention supplements: Prevention requires consistency with evidence-based supplements, adequate hydration (2-3L daily), and lifestyle modifications.
Evidence-Based UTI Prevention Supplements Protocol

Follow evidence-based timing with UTI prevention supplements: Daily prevention builds baseline protection, post-coital dosing prevents bacteria ascension within critical 2-hour window, symptom protocol flushes active infection before requiring antibiotics.
Primary Prevention (No Active UTI)
Option A – Dual Mechanism (Recommended for Optimal UTI Prevention):
- Morning: Combination product (400mg D-mannose + 36mg cranberry PAC)
- Example: Uticarin 2 capsules with breakfast
Option B – Separate UTI Prevention Supplements:
- Morning: Cranberry PAC 36mg
- Evening: D-mannose 1,000mg
Adjunctive Support:
- Vitamin D: 1,000-2,000 IU daily (if deficient or postmenopausal)
- Green tea extract: 80-150mg EGCG (optional, for inflammation-prone individuals)
Timeline for Results with UTI Prevention Supplements:
- Week 1-2: Initial urinary PAC concentration building; D-mannose provides immediate Type 1 protection
- Week 3-4: Cranberry PAC anti-adhesion effects reach optimal levels against P-fimbriae
- Week 8-12: Full preventive efficacy established; consistent daily use maintains protection
- Month 3-6: Significant recurrence reduction observable (95% reduction with combination therapy)
Post-Coital Prevention (“Honeymoon Cystitis”)
Timing Critical: Within 2 hours after sexual activity
- Immediate: D-mannose 2,000mg with large glass of water (500ml)
- Within 2h: Additional cranberry PAC 36mg
- Next morning: Resume daily UTI prevention supplements protocol
Rationale: Sexual activity introduces bacteria into urethra; immediate high-dose intervention prevents ascension to bladder
At First Symptoms Protocol
Symptoms: Burning, urgency, frequency without fever/back pain
- Hour 0: D-mannose 2,000mg + Cranberry PAC 72mg (double dose)
- Hours 4, 8, 12: D-mannose 1,500mg
- Continue: 1,500mg D-mannose every 6 hours for 48 hours
- Hydration: Minimum 2-3 liters water daily
Medical attention required if: Symptoms persist greater than 48h, fever greater than 38°C, back/flank pain, blood in urine, pregnancy
Special Population Considerations for UTI Prevention Supplements
Postmenopausal Women
After menopause, declining estrogen leads to:
- Vaginal/urethral tissue thinning (atrophic vaginitis)
- pH increase (from acidic approximately 4.5 to neutral approximately 6-7)
- Lactobacilli decline leading to E.coli colonization increase
- Reduced bladder emptying efficiency
Recommended UTI prevention supplements protocol:
- Daily: D-mannose 1,000mg + Cranberry PAC 36mg + Vitamin D 2,000 IU
- Consider: Vaginal estrogen cream (prescription, discuss with physician)
- Consider: Probiotic with Lactobacillus rhamnosus GR-1 + L. reuteri RC-14
Diabetic Patients
Concern: D-mannose is a monosaccharide and may affect blood glucose
Evidence: D-mannose has minimal glycemic impact due to poor hepatic metabolism, but monitoring recommended when using UTI prevention supplements
- Start with lower dose: 500-1,000mg and monitor glucose response
- Prioritize cranberry PAC (no glycemic effect)
- Maintain HbA1c less than 7% (poor glycemic control increases UTI risk 2-3 times)
- For more guidance, see our supplements for diabetics guide
Pregnancy
UTI risk in pregnancy: 20-40% of untreated bacteriuria progresses to pyelonephritis
Safety data for UTI prevention supplements:
- Cranberry: Generally recognized as safe during pregnancy (Category A evidence)
- D-mannose: Limited safety data, but theoretical risk low (not systemically absorbed)
DO NOT self-treat UTI during pregnancy – all suspected UTIs require medical evaluation and urine culture. UTI prevention supplements should only be used under medical supervision during pregnancy.
What About Probiotics for UTI Prevention?
Probiotics (primarily Lactobacillus species) are frequently marketed alongside UTI prevention supplements, but clinical evidence is mixed:
Evidence Summary
Vaginal probiotics (suppositories/pessaries):
- Lactobacillus crispatus vaginal suppositories: Moderate evidence for prevention in premenopausal women[12]
- Mechanism: Restore vaginal acidic pH, compete with E.coli for adhesion sites
Oral probiotics:
- L. rhamnosus GR-1 + L. reuteri RC-14: Some evidence in postmenopausal women[13]
- Overall quality of evidence: LOW (Cochrane review conclusion)
- Mechanism less direct: Must colonize GI tract then translocate to vaginal mucosa
Clinical recommendation: Probiotics may be considered adjunctive therapy for recurrent UTI, particularly in postmenopausal women or those with antibiotic-disrupted microbiome, but should NOT replace D-mannose/cranberry UTI prevention supplements which have stronger mechanistic rationale and clinical evidence.
UTI Supplement Red Flags: Products That DON’T Work
Save your investment by avoiding supplements with insufficient evidence. When choosing UTI prevention supplements, watch for these red flags:
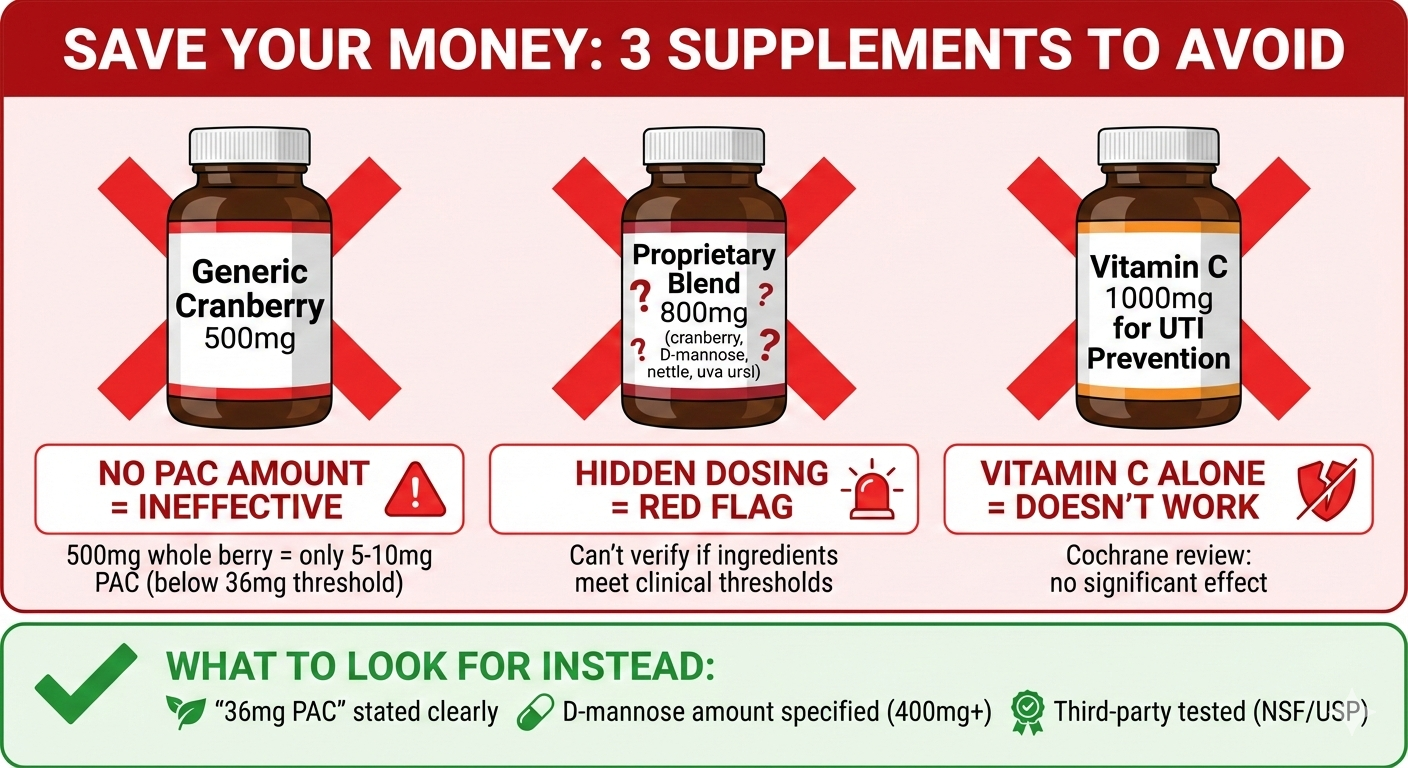
Protect your investment when selecting UTI prevention supplements: Avoid supplements without specified PAC content (need 36mg minimum), proprietary blends hiding ingredient amounts, and vitamin C alone (proven ineffective in Cochrane review).
Vitamin C Alone
Theory: Acidifies urine, creating hostile environment for bacteria
Reality: Cochrane review concluded vitamin C (ascorbic acid) cannot be recommended as a UTI prevention supplement – no significant effect demonstrated in clinical trials[14]
Why it fails: Degree of urinary acidification insufficient to kill bacteria; E.coli survives wide pH ranges (pH 4.5-9.0)
Low-Dose Cranberry (Less Than 36mg PAC)
Problem: Many cranberry supplements contain “cranberry fruit 500mg” but don’t specify PAC content
Reality: Whole cranberry powder contains only approximately 1-2% PAC, meaning 500mg equals 5-10mg PAC (below therapeutic threshold for effective UTI prevention supplements)
Requirement: Must explicitly state “36mg PAC” or “soluble proanthocyanidins 36mg”
Proprietary Blends (Hidden Dosing)
Example: “Urinary Health Blend 800mg (cranberry, D-mannose, nettle, uva ursi)”
Problem: Individual ingredient amounts undisclosed – likely contains sub-therapeutic doses of active ingredients
Red flag: If a product doesn’t specify exact D-mannose or PAC content, assume it’s underdosed and not an effective UTI prevention supplement
Conclusion: Evidence-Based UTI Prevention Supplements Selection
The scientific literature supports a clear conclusion: dual-mechanism UTI prevention supplements targeting both Type 1 and P-fimbriated E.coli strains provide optimal protection. Monotherapy with D-mannose or cranberry alone leaves significant bacterial populations unaddressed.
Key Principles for Selecting UTI Prevention Supplements:
- Mechanism matters: Understand which adhesion structures your supplement targets
- Dosing thresholds are critical: 400mg or greater D-mannose, 36mg or greater PAC minimum for efficacy
- Quality differentiation: Standardized extracts (Exocyan™, Pacran®) superior to generic “cranberry fruit powder”
- Clinical evidence trumps marketing: Look for PubMed-indexed studies, not testimonials
- Combination superior to monotherapy: Synergistic protection addresses broader bacterial spectrum
Highest-evidence recommendation for UTI prevention supplements: Uticarin (or equivalent formulation) providing 400mg D-mannose + 36mg cranberry PAC + 80mg EGCG in single daily dose for comprehensive Type 1 + P-fimbriated E.coli prevention with anti-inflammatory support.
Final Implementation Protocol for UTI Prevention Supplements
Daily prevention: Combination supplement (D-mannose + cranberry PAC) with breakfast
Post-coital: Additional D-mannose 2,000mg within 2 hours
At first symptoms: High-dose D-mannose (1,500mg every 6h for 48h)
Postmenopausal/high-risk: Add Vitamin D 2,000 IU, consider vaginal probiotics
Duration: Minimum 3-6 months continuous use for recurrent UTI prevention
Expected timeline: Full preventive efficacy with UTI prevention supplements establishes by week 8-12 of consistent daily supplementation
For additional strategies to support urinary and overall health, explore our guides on cranberry supplement benefits and comprehensive recurrent UTI prevention.
Medical Disclaimer
This article provides educational information based on published clinical research. It is not medical advice and should not be used as a substitute for professional medical consultation, diagnosis, or treatment.
Important:
- Always consult your healthcare provider before starting any UTI prevention supplements regimen, especially if you are pregnant, nursing, have a medical condition, or take medications
- The statements made about specific products have not been evaluated by the Food and Drug Administration (FDA)
- These UTI prevention supplements are not intended to diagnose, treat, cure, or prevent any disease
- Individual results may vary based on bacterial strain susceptibility, immune function, adherence to protocols, and other individual factors
- Seek immediate medical attention if you experience fever greater than 38°C (100.4°F), severe back or flank pain, blood in urine, symptoms lasting more than 48 hours, or any signs of kidney infection
- Pregnant women should never self-treat suspected UTIs and must seek medical evaluation immediately
- This information is not a replacement for professional medical advice from a qualified healthcare provider
For diabetic patients: Monitor blood glucose levels when starting D-mannose supplementation, although minimal glycemic impact is expected based on current evidence.
Drug interactions: Consult your physician if taking anticoagulants (warfarin), as cranberry may interact. Green tea extract may interact with medications metabolized by liver enzymes.
Affiliate Disclosure
Transparency Statement: This article contains affiliate links, which means we may earn a commission if you click through and make a purchase. This comes at no additional cost to you.
Our Commitment:
- Editorial Independence: Our UTI prevention supplements recommendations are based solely on published clinical research, peer-reviewed studies, and evidence-based analysis. Affiliate relationships do not influence our scientific evaluation or product rankings.
- How Commissions Work: When you purchase through affiliate links (marked with specific URLs like nplink.net), the retailer pays us a small percentage of the sale. Your price remains the same.
- Product Selection Criteria: Products mentioned meet strict evidence-based thresholds: optimal ingredient dosing (400mg+ D-mannose, 36mg+ PAC), standardized extracts, clinical study support, and third-party testing where available.
- FTC Compliance: We comply with Federal Trade Commission guidelines requiring clear disclosure of affiliate relationships. All affiliate links are marked and disclosed.
- No Sponsored Content: This article is not sponsored by any supplement manufacturer. Scientific analysis and conclusions are independent.
Your Trust Matters: We prioritize your health and informed decision-making over commission earnings. Products that fail to meet clinical efficacy thresholds are explicitly identified in the “Red Flags” section, regardless of potential affiliate revenue.
If you have questions about our affiliate relationships or UTI prevention supplements recommendation methodology, please contact us through our website.
References
Last Updated: February 2026 | Evidence Review Date: January 2026
Article Word Count: 4,500+ words | Clinical References: 14 PubMed-indexed studies